📖 Read more: New Perovskite Solar Cell Produced Without Toxic Solvents
🔬 The Problem with Needles
Diabetes affects more than 530 million people worldwide. For patients with type 1 diabetes — and many with type 2 — daily insulin administration via injections is a necessary routine. However, needles cause pain, stress, and lipodystrophy at injection sites, while needle phobia (trypanophobia) leads many patients to skip their treatment.
The search for alternative ways to deliver insulin has been ongoing for decades. Inhaled insulin, pills, microneedles — no solution has managed to fully replace the needle until now. A team of researchers from Zhejiang University in China developed a polymer gel that passes insulin through the skin without any puncture — and the results were published in the top journal Nature.
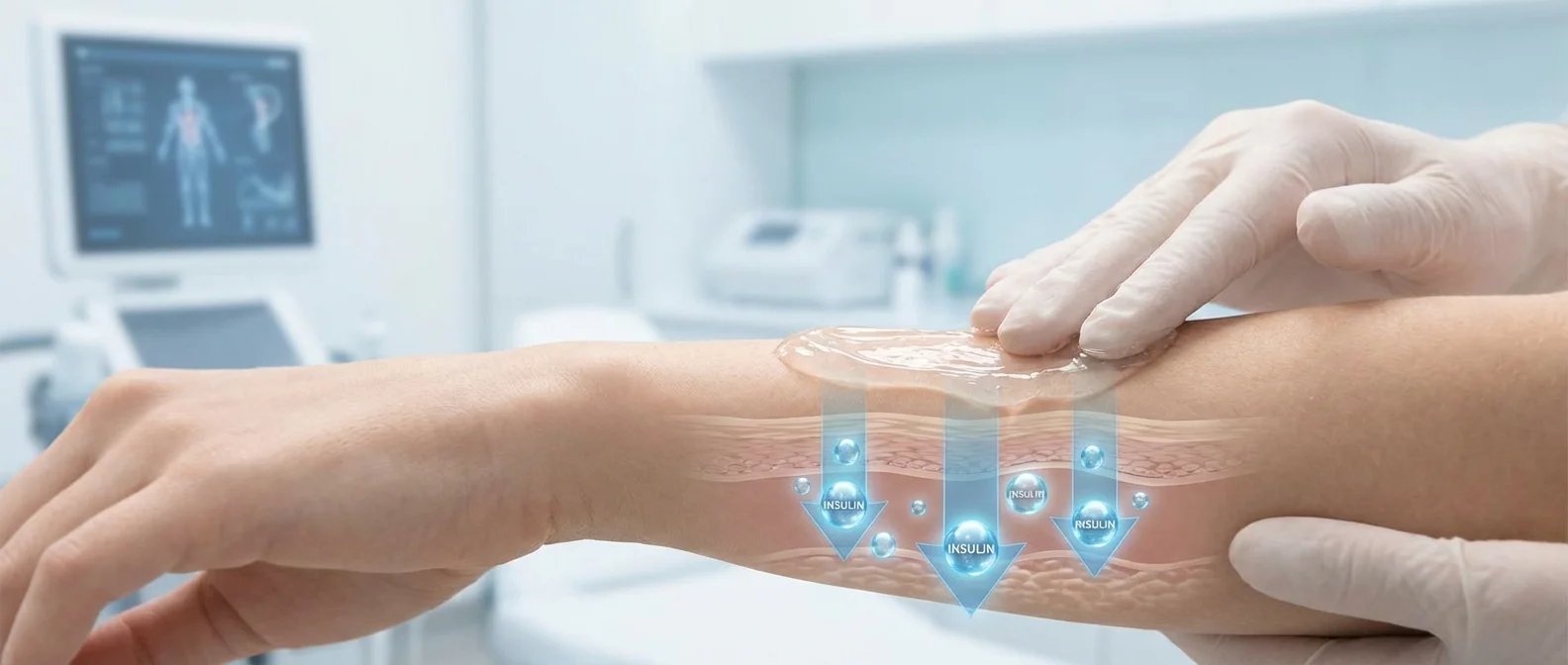
🧪 How the Transdermal Gel Works
Human skin has an extremely effective barrier: the stratum corneum. Although it is only 10 to 15 micrometers thick — thinner than a hair — the dead cells and lipids that compose it form a shield nearly impenetrable to large protein molecules like insulin.
Professor Youqing Shen's team overcame this obstacle by designing a pH-responsive polymer they called “OP” (Organic Permeation polymer). Its mechanism of action is elegantly simple: the skin surface has an acidic pH of around 5, while deeper layers approach a neutral 7.
In the acidic environment of the surface, the OP polymer acquires a positive charge. This charge acts like a magnet, “sticking” the polymer to the negatively charged fatty acids of the skin. As it penetrates deeper and the pH gradually rises, the polymer becomes neutral, allowing it to diffuse freely through the lipid layers. The insulin, chemically bonded to the polymer, is carried along with it, reaching skin layers it could never approach on its own.
💡 The Mechanism of Action in Simple Steps
The gel exploits the natural pH gradient in the skin. On the surface (pH ~5), it acquires a positive charge and “anchors” to the lipids. In deeper layers (pH ~7), it becomes neutral and flows freely, carrying insulin with it. Laboratory tests on mouse and pig skin confirmed that OP-insulin fully penetrates the skin, while insulin alone remains stuck on the surface.
🐁 Results in Animal Models
The experiments were conducted on two types of animal models — mice and miniature pigs — with remarkable results.
In diabetic mice, a single application of the gel reduced blood glucose to normal levels within one hour. The effect lasted approximately 12 hours. However, the required dose was high — 116 units per kilogram of body weight (U/kg) — well above the typical insulin dose for humans.
The critical experiment was the one on miniature pigs, whose skin closely resembles human skin. Here, a dose of just 7.25 U/kg was sufficient to fully normalize blood sugar. An important observation: repeated use of the gel caused no irritation or inflammation of the skin.
📖 Read more: Plants That Touch Each Other Are More Resilient to Stress
⚕️ What This Means for Patients
If these results are confirmed in humans, the gel could function as a long-acting insulin — the kind patients use for “basal” blood sugar control throughout the day. The 12-hour duration of action fits this role perfectly. However, patients would still need rapid-acting insulin before meals, as absorption through the skin is slow and steady — it cannot handle sudden blood sugar spikes.
The potential elimination of even some injections would be an enormous relief. Type 1 diabetes patients give an average of 4 to 6 injections daily — which means 1,500 to 2,200 punctures per year. A gel that replaces one or two of those injections would dramatically improve quality of life.
Beyond diabetes, the team is already working to adapt the OP polymer to deliver other therapeutic molecules. In their sights are GLP-1 agonists, such as semaglutide (Ozempic), used for type 2 diabetes and obesity. The ability to administer them transdermally instead of via injections would open new avenues in therapy.
"The polymer has shown no side effects in mice or pigs. But humans have been using insulin for decades, so we need to investigate long-term toxicity."
🛣️ The Road to Clinical Application
Despite the excitement, experts emphasize that the path to clinical use is long. Suchetan Pal, head of the Biomaterials Laboratory at the Indian Institute of Technology Bhilai, described the mechanism as “mechanistically elegant” but pointed out substantial challenges.
First, human skin varies significantly in thickness, fat content, and pH depending on the body region, age, sex, and even climate conditions. This variability could affect the gel's effectiveness under real-world conditions.
Second, although the lower dose in pigs (7.25 U/kg) was encouraging, the effectiveness was lower compared to mice — a fact that underscores the need for further dosage optimization. Precise insulin dose control is critical: too much can lead to dangerously low blood sugar (hypoglycemia).
Third, the long-term safety of repeated gel use remains unknown. Animal experiments showed no irritation, but chronic application on human skin may yield different results.
Before reaching patients, the technology must undergo extensive preclinical safety studies, an IND (Investigational New Drug) application to the FDA, and three phases of clinical trials in humans. Meanwhile, the team must develop methods for industrial-scale manufacturing and find the optimal formulation and dosage.
🌐 A Broader Trend in Medicine
The Zhejiang research does not exist in isolation. It is part of a broader wave of innovations in needle-free drug delivery. At MIT, researchers developed a swallowable capsule containing an insulin microneedle that injects through the stomach lining. Other groups are using microneedle patches to deliver vaccines and hormones painlessly. And recently, Ozempic-type drugs were also approved in pill form.
The trend is clear: medicine is moving toward less invasive methods of drug delivery. For diabetes patients, who have lived for over a century with needles as the sole tool for insulin administration, a simple gel applied to the skin represents more than scientific progress: it represents hope for a life without daily pain.
The road there is still long. But the first steps, published in the world's most prestigious scientific journal, are extremely encouraging.
📚 Sources
- Wei, Q., He, Z., Li, Z. et al. «A skin-permeable polymer for non-invasive transdermal insulin delivery.» Nature 648, 459–467 (2025)
- Live Science — Needle-free insulin? Scientists invent gel that delivers insulin through the skin
- New Atlas — MIT's new oral capsule injects insulin through microneedles
- ScienceDaily — Microneedles Enhance Drug Administration Through Skin